At the SCDM Annual Conference in 2023, I had the privilege of chairing a panel, Are you ready for EHR eSource? Lessons from the field. Three esteemed panelists joined me:
- Adam Asare, Chief Data Officer, Quantum Leap Healthcare Collaborative
- Mike Hogarth, Clinical Research Information Officer, UCSD Health
- Dan Hydes, CEO, IgniteData
Allow me to share my highlights from our insightful conversation.
-
- Regulators like the FDA encourage the exchange of structured data such as demographics, vital signs and lab data between the EHR and EDC systems so data can be entered once at the point of care use, many times without manual reentry or manual source data verification.
- There are trends that are building momentum for eSource, including:
- Modern standards such as FHIR and SMART on FHIR,
- Data quality and consistency across sites,
- Control in the hands of sites and patients,
- Frameworks for access and protection of privacy,
- Increased focus on real-world evidence (RWE) for research,
- Regulatory mandates such as the ONC,
- Much faster and more accurate than CRF-based transcription
- There is ample reliable and compelling evidence EHR eSource integration works.For an adaptive platform trial of repurposed therapeutics for patients hospitalized with a severe infectious disease, the use of eSource technology resulted in significant time and cost savings, including:
- A 16-minute per form savings for elapsed data entry time on the primary daily eCRF, a 61 percent reduction compared to manual entry;
- For just 52 patients studied at one site (UCSF) with a 15-day treatment course, 208 hours of clinical research coordinator time was saved;
- The elimination of data errors by the automated, validated EHR-loaded data and the downstream costs associated with cleaning, source data verification (SDV) and validation;
- Low implementation costs, and
- Reusability across sites.Dan Hydes of IgniteData recounted his organization’s experience with an oncology study at the University College London Hospital. The study had 900 patients and included 20 visits per patient.
“The manual data transfer took approximately three minutes, totaling 68.7 hours to enter data manually for 20 visits.”
The use of EHR-to-EDC resulted in a savings of nearly 67 hours per patient. For 900 patients, that’s more than 60,000 hours.

- It’s simple and quick to implement EHR eSource integration. As Adam Asare of Quantum Leap Healthcare Collaborative noted,
“None of these sites had actually done this work before directly for an EHR to EDC capture, and these are all the sites listed here. And they were able to get this up in an average of two to three weeks [at the height of the COVID-19 pandemic.]”
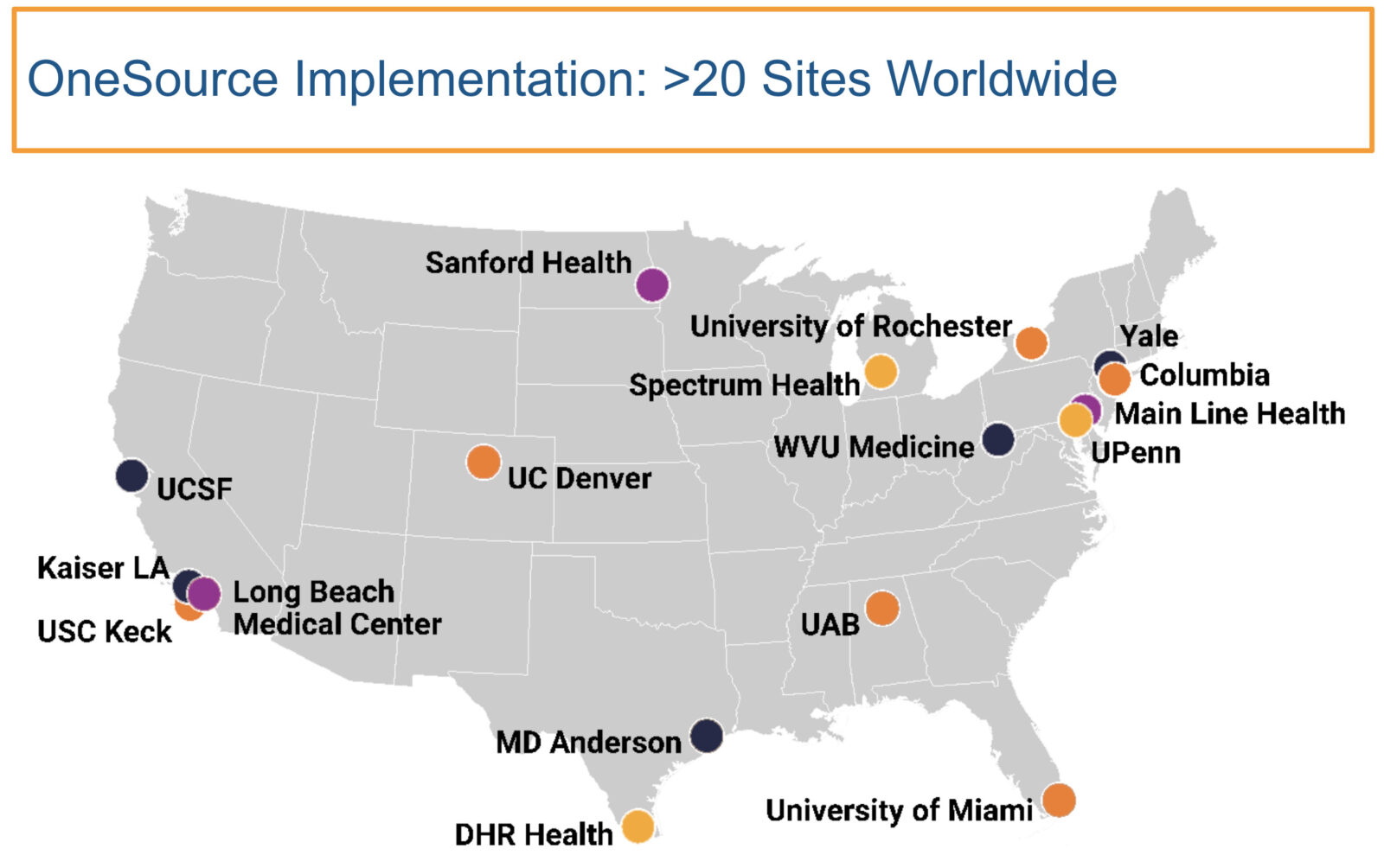
- Champions facilitate site adoption of EHR eSource. Asare of Quantum Leap Healthcare Collaborative shared,
“We discovered what we had to do was prove why this was important, and to do so, we had to find the champion at the site. Not only the investigator, but the clinical research coordinators had to really be very vocal and say they wanted [eSource].”
He also noted that community centers required a clinical champion.
Dan Hydes of IgniteData added that sites needed outside implementation resources,
“Sites say we absolutely want this. But we haven’t got any staff really to work on deploying this. Can you come with a paying study from a sponsor that will fund that small piece of implementation?”
Likewise, the IT Department needs to buy-in. Mike Hogarth of UCSD emphasized,
“Convincing the IT department that this is a priority is critical.”
He suggested using his test which demonstrated in 29 minutes they
“had a test record being pulled from the middleware pipe system using FHIR.”
For more on why to prioritize EHR eSource integration, read my recent blog, 2024: The Year of EHR eSource in Clinical Trials.



